If you experience digestive symptoms, especially in the upper digestive system, you may have a bacterial infection called Helicobacter pylori (H. Pylori).
Do the following sound familiar? Burning pain in the abdomen, bloating/ burping after eating, bad breath, nausea, aversion to meat, loss of appetite, weight loss. If you have any of these symptoms, you may want to rethink just simply turning to Tums or avoiding food triggers (caffeine, tomatoes, chocolate, alcohol, spicy foods).
Why Test?
H. Pylori is the only bacteria classified as a carcinogen because if left untreated it can progress to cancer and other issues like Barrett’s Esophagus and autoimmune conditions such as Hashimoto’s and Rheumatoid Arthritis. According to CDC 80% of stomach ulcers are due to H. Pylori. Worse yet, one study showed 46% of individuals who experience GERD (reflux) were infected with H. Pylori.
H. Pylori is diagnosed through a couple of ways: blood (serum), breath, and stool. The problem with testing is that blood (antibody) testing is typically only accurate during initial stages of infection. Meaning that this type of testing completely misses those who are chronically infected. The other issue is not all strains of H. Pylori are “bad” or “pathogenic” meaning the potential to cause disease.
How Does H. Pylori Create Disease?
The exact way H. pylori infects someone is still unknown. H. pylori bacteria may be passed from person to person through direct contact with saliva, vomit or fecal matter. H. pylori may also be spread through contaminated food or water. The principal risks for developing H. Pylori include poor hygiene (here is a reference), and a diet with low fruit and vegetable intake. Research has also found that there is a link of psychological stress to the development of H. pylori.
Once a person is infected, H. pylori burrows down into and attacks the lining that protects your stomach. H.pylori also starts to make an enzyme called urease. This enzyme makes your stomach acids less acidic (neutralizes them by converting urea to ammonia). This weakens your stomach’s lining makes it more susceptible to being hurt by acid and pepsin that leads to ulcers in the stomach and small intestine.
At the beginning of active H. pylori infection, people may experience hypochlorhydria (low hydrochloric acid (HCL) production) followed by a shift to hyperaciduria (high acidity in the urine). This is why I sometimes also check urine pH levels.
If H. Pylori neutralizes or lowers stomach acid, why does someone still get heartburn?
Normally stomach acid is very acidic. If the stomach is not acidic, the stomach contents do not empty properly and the lower esophageal sphincter or LES does not close to prevent reflux from the stomach from going up into the esophagus.
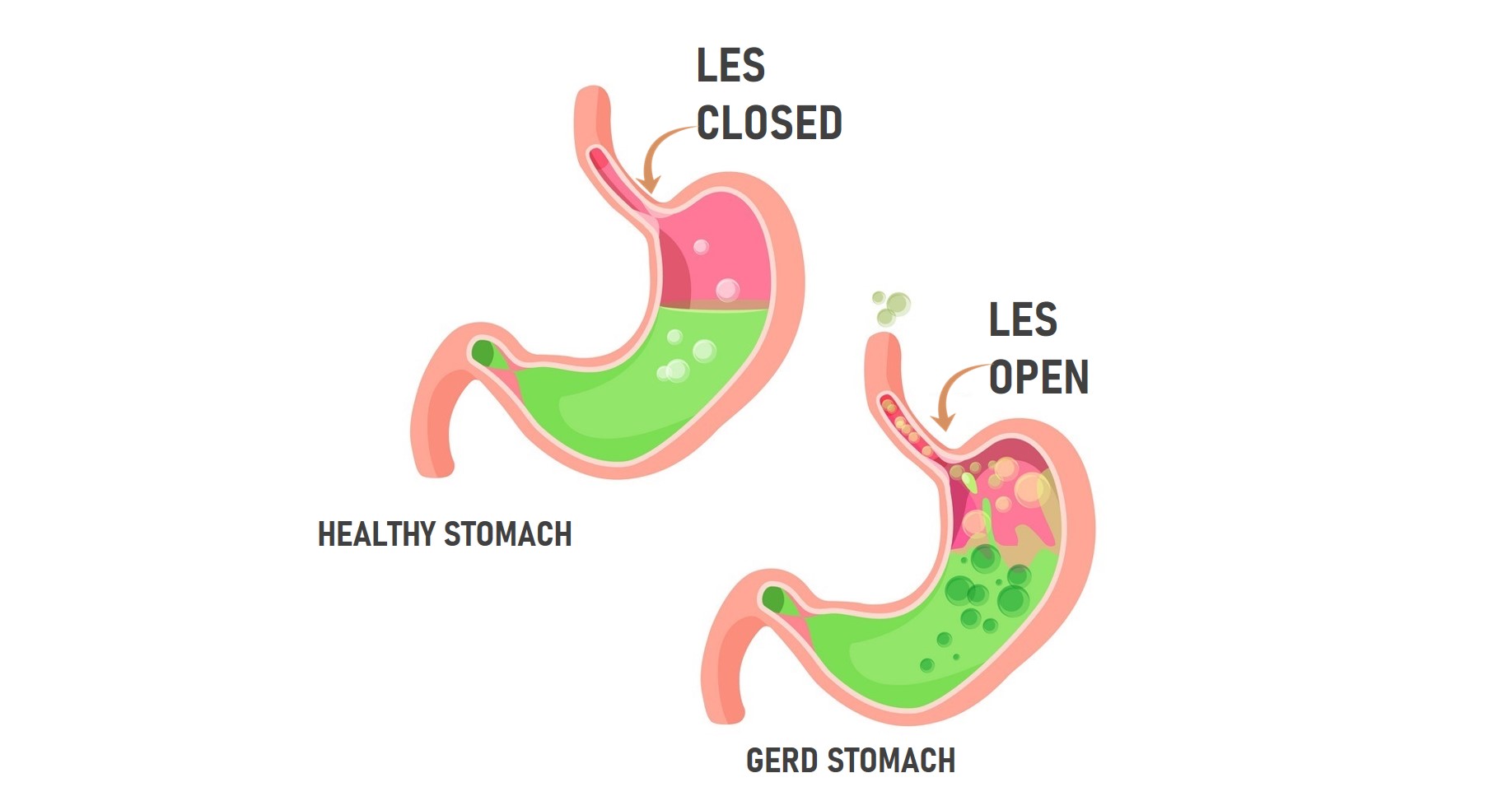
The food sits in the stomach and is fermented by bacteria into lactic acid. The lactic acid produces the “burn” pain you feel (same as when you exercise). Proton pump inhibitors or PPIs may produce symptom relief but as you will see in this article they do not address the root cause and the risk (especially nutrient deficiencies) often outweighs the benefits.
In conclusion, if the stomach acid does not get to the proper acidity level, problems start to arise.
Symptoms: due to low stomach acid or hypochlorhydria, due to H. pylori or as a result of PPI (Nexium) or H2 Receptor Blocker (Zantac) use
- Nutrient deficiencies: malabsorption of minerals like calcium, magnesium, iron, zinc, copper, selenium and boron. Many are necessary for thyroid function, magnesium is a cofactor for over 300 reactions, zinc for 250 reactions. Minerals are needed for bone health.
- Anemia: If you have a chronic iron deficiency and don’t know why – look for gut infections.
- Fatigue: Vitamin B12 and folate are important for energy and neurotransmitters
- Protein deficiency: Inability to digest and absorb protein meaning less building blocks for tissue repair
- Gall bladder issues: low stomach acid stimulates CCK and secretin to be released. CCK tells the gallbladder to squeeze and release bile to promote bowel motility. Secretin tells the liver to refill the gallbladder. Bile is necessary to breakdown and absorption of fats.
- Hormone imbalance: The cholesterol in fats is used to make hormones. If we don’t break down fats properly, we risk having imbalanced hormones.
- Less stomach acid increases the risk for SIBO (small intestinal bacterial overgrowth)
- Bloating
- Burping
- Gas
- Diarrhea (or constipation)
- Hair loss
- Skin Problems (ex. Rosacea – see below)
- Weak nails
- Intestinal infections (like worms & parasites)
- Nausea while taking supplements
- Undigested food in the stool
- Food sensitivities
There is also a link between hypochlorhydria and several other medical issues, such as:
– allergies
– asthma
– autoimmune disorders
– skin problems, including acne and psoriasis
H. Pylori and The Skin
New high quality research is coming out on the relationship between H. Pylori and a common skin condition called Rosacea. This is an inflammatory skin condition that causes redness, pimples and visible blood vessels to appear. It most commonly affects the cheeks, nose and eyes. Like acne, rosacea can cause significant social stigmatization and worsen quality of life. It increases the risk of depression and mental health issues.
While researchers don’t fully agree on whether a relationship exists, most studies suggest one does. Further, treatment of H. Pylori can improve the symptoms of rosacea. In some studies even more so than medications designed to treat rosacea.
How is H. pylori diagnosed?
Your healthcare provider will look at your past health and give you a physical exam. He or she may also use any of these available tests (listed from most accurate to least accurate):
Stomach Biopsy: Upper endoscopy, also called EGD (esophagogastroduodenoscopy). This test is the most accurate but is the most INVASIVE and requires a specialist appointment. It looks at the lining of your food pipe (esophagus), stomach, and duodenum (the first part of your small intestine). It uses a thin, lighted tube or endoscope. The tube has a camera at one end. The tube is put into your mouth and throat. Then it goes down into your esophagus, stomach, and duodenum. Your healthcare provider can see the inside of these organs. A small tissue sample (biopsy) is taken and the tissue sample can show if you have the enzyme urease. It can also check the bacteria that is there. As you can imagine, this isn’t the most pleasant procedure and doesn’t come without its risks. It’s also not the preferred testing method for those under the age of 50 and with those without alarm features.
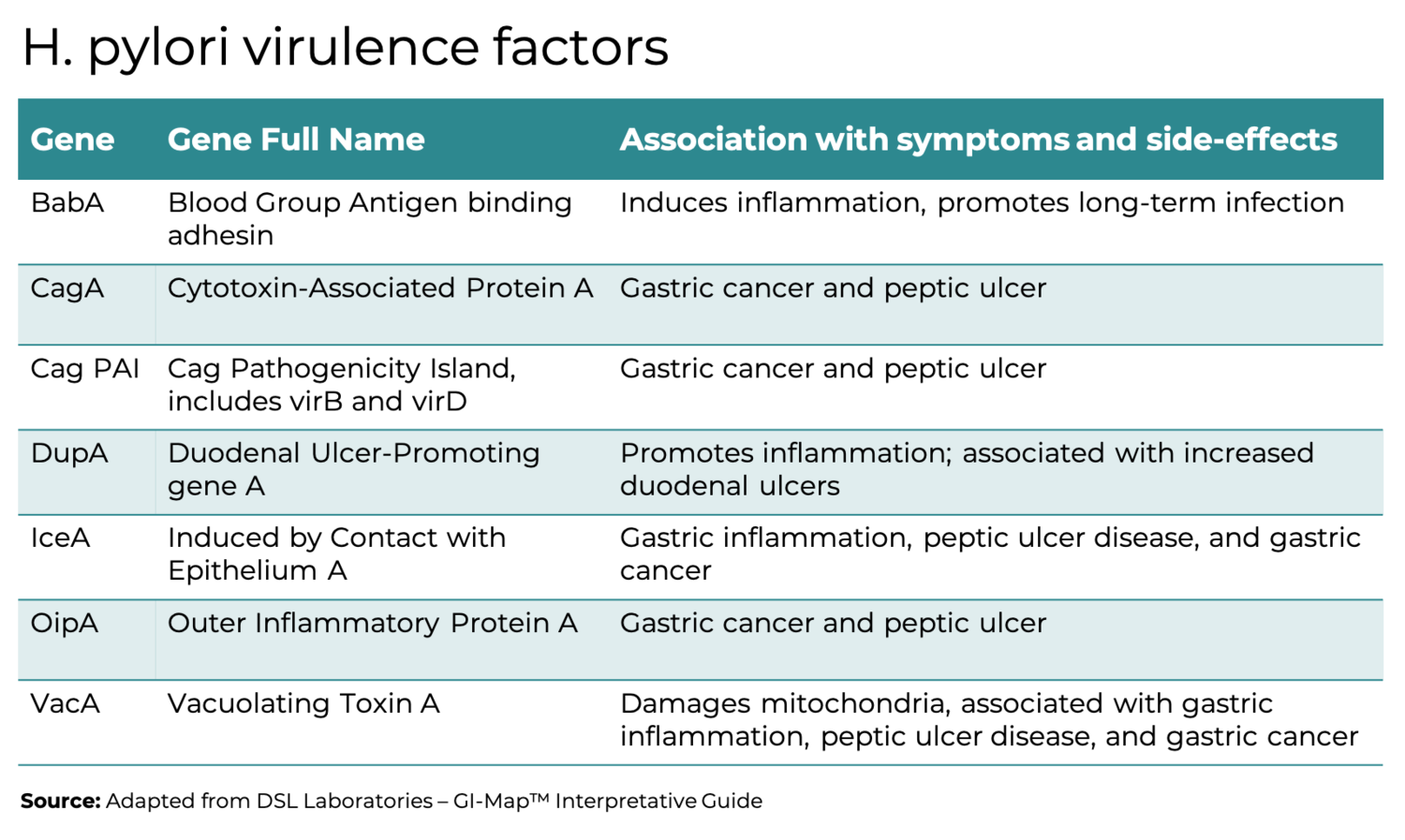
PCR Technology Stool analysis (most preferred, non invasive, new on the market, least difficult). The GI MAP by Diagnostic Solutions test is a stool test that looks for any abnormal bacteria in your digestive tract, normal bacteria, worms, parasites, digestive function, and more. The doctor gives you a stool kit, you collect a small stool sample at home, and send it off with a pre-paid postage label to the lab. Test results come back in 5-7 days. This test not only tells you if you have H. Pylori, but also gives insight into its virulence factors. The two most well known virulence factors are the cagA and VacA genes. They are responsible for the cancer-causing and ulcer- forming effects of chronic H. pylori infection. This test can also identify other co-infections that may be contributing to GI symptoms.A sample report can be seen here.

Breath test (non invasive, difficult to perform). This test must be done in a lab, takes a few hours and requires preparation. During the test, you will drink a solution of swallow a capsule that contains urea and samples of your breath are collected. If H. Pylori is present, the isotope carbon in the exhaled carbon dioxide will be detected in your breath sample. If carbon is found that means that H. pylori has made the enzyme urease. This enzyme makes your stomach acids less acidic and weakens your stomach’s mucous lining. Test prep instructions can be found here.
Blood antibody test (most common, least accurate). This test checks to see if your body has made antibodies to H. Pylori bacteria. If you have antibodies to H. pylori in your blood, it means you either are currently infected or have been infected in the past. It often misses chronic infections.
Why? This is because H pylori secretes a lipopolysaccharide (LPS) called lewis antigens. These help the H. pylori “hide” from the immune system and divert the attack too often the parietal cells. Parietal cells of the stomach secrete hydrochloric acid and intrinsic factor. Intrinsic factor is necessary for absorbing B12. These lipopolysaccharides have been linked to autoimmune diseases such as type 1 diabetes, rheumatoid arthritis and Hashimoto’s thyroiditis.
Bottom line: the best test for H. Pylori is the GI MAP stool test. It is highly sensitive and specific and it shows virulence factors for H pylori (how likely is it to create disease). The GI MAP test also shows antibiotic resistance genes for H.pylori to provide insight into whether or not antibiotic therapy would be effective as well as which antibiotics would be the most effective.
How is H. Pylori Treated?
1) Antibiotics
The traditional medical approach utilizes triple therapy as the first-line of treatment which consists of a proton pump inhibitor (PPI), and antibiotics clarithromycin and amoxicillin for 7-14 days. However, the effectiveness in eliminating H. pylori infections is lower than 70%, mainly due to the antibiotic clarithromycin resistance. They are no longer considered gold standard. Also, antibiotic therapy reduces your friendly bacteria leaving your microbiome unbalanced which can lead to new infections and ongoing chronic health issues. It can also cause antibiotic associated diarrhea.
2) Natural treatment for H. Pylori
Tailored natural antimicrobials along with supportive nutrition, probiotics, anti-inflammatories that promote tissue healing. There are hundreds of scientific publications worldwide that describe accurately the antibiotic activity of herbal products for H. pylori. (Reference)
Additional testing including food sensitivities, SIBO, and organic acid test that assesses the microbial, mitochondrial, nutritional, and detox burdens all may be considered to investigate the potential causes of digestive concerns further.
Final thoughts
H. pylori infection is very common and often under-looked, especially when you don’t have digestive symptoms. It can cause stomach cancer, chronic inflammation of the stomach and ulcers if left untreated. Taking antacids and PPI medications is not enough.
If you or a loved one has gone through several rounds of unsuccessful treatment, don’t give up. If you have just been diagnosed, then you should consult with a naturopathic doctor who can help you increase treatment success while reducing side effects.
PS…
Did you know Zantac (Ranitidine) has been recalled in October 2019? Please if you are still on this medication, talk to your doctor. Read your medication inserts for drug prescriptions! Ranitidine specifically says “Do not take over-the-counter ranitidine for longer than 2 weeks”. Nexium reads “NEXIUM is indicated for the short-term treatment (4 to 8 weeks) “. If you are on these medications longer than that, ask yourself why?! “Proton pump inhibitor treatment should only be initiated and continued if the benefits outweigh the risks of treatment”.
I recommend a free 10-15 minute introductory call or in-person consultation with me to see if a naturopathic assessment for H. Pylori may be right for you. Please keep in mind that naturopathic consultations are covered by extended health care plans.
To book an appointment with me:
-Dr Diana Semjonov, ND
Note: Testing may be covered under healthcare insurance. Check with your provider. If needed, costs can be discussed during an intro call.
This article is for educational purposes only and does not advocate self-diagnosis. Due to individual variability, consultation with a licensed health professional, such as a naturopathic physician is highly recommended prior to starting a natural treatment plan.
References:
Jung, Da Hyun, and Hyojin Park. “Is Gastroesophageal Reflux Disease and Achalasia Coincident or Not?.” Journal of neurogastroenterology and motility vol. 23,1 (2017): 5-8.
Kountouras, Jannis et al. “Potential implications of Helicobacter pylori-related neutrophil-activating protein.” World journal of gastroenterology vol. 18,5 (2012): 489-90.
Pohl, Daniel et al. “Review of current diagnostic methods and advances in Helicobacter pylori diagnostics in the era of next generation sequencing.” World journal of gastroenterology vol. 25,32 (2019): 4629-4660.
El-Eshmawy, Mervat M et al. “Helicobacter pylori infection might be responsible for the interconnection between type 1 diabetes and autoimmune thyroiditis.” Diabetology & metabolic syndrome vol. 3,1 28. 26 Oct. 2011.
https://www.uspharmacist.com/article/proton-pump-inhibitors-considerations-with-longterm-use
https://www.accessdata.fda.gov/drugsatfda_docs/label/2014/022101s014021957s017021153s050lbl.pdf
Park, Ji Sook et al. “Gastric autoantigenic proteins in Helicobacter pylori infection.” Yonsei medical journal vol. 54,6 (2013): 1342-52.
Sterzl, I et al. “Anti-Helicobacter Pylori, anti-thyroid peroxidase, anti-thyroglobulin and anti-gastric parietal cells antibodies in Czech population.” Physiological research vol. 57 Suppl 1 (2008): S135-41.
Papamichael, Konstantinos X et al. “Helicobacter pylori infection and endocrine disorders: is there a link?.” World journal of gastroenterology vol. 15,22 (2009): 2701-7.
Kusters, Johannes G et al. “Pathogenesis of Helicobacter pylori infection.” Clinical microbiology reviews vol. 19,3 (2006): 449-90.
Ayala, Guadalupe et al. “Exploring alternative treatments for Helicobacter pylori infection.” World journal of gastroenterology vol. 20,6 (2014): 1450-69.
Jørgensen, A‐HR, et al. “Rosacea is associated with Helicobacter pylori: a systematic review and meta‐analysis.” Journal of the European Academy of Dermatology and Venereology 31.12 (2017): 2010-2015.
0 Comments Leave a comment