Calcium is an essential mineral for good health. Particularly bone health, as 99% of all calcium in the body is found in bone and teeth. This is a nutrient we need in the highest quantities but also has the highest chance of being harmful. In this article, I will guide you into determining if you need to supplement calcium, how to supplement and in which form.
The major benefit of calcium intake is preventative in reducing the risk of developing osteoporosis during the aging process. As a reminder, osteoporosis occurs when you lose too much bone or don’t make enough bone to begin with. Women are more predisposed than men because they naturally have lower bone mass, which is further diminished by lower hormone levels after menopause. In severe osteoporosis, even a minor fall can cause a bone fracture. A fracture of the hip in particular can lead to severe complications and a significant demise in quality of life. Ensuring adequate calcium levels throughout life can prevent this.
Now let’s go on to look at the evidence for calcium supplementation.
Latest research claims that supplementing calcium ALONE to prevent bone mineral density loss and prevent fractures is not recommended. Here are the reasons why:
1. Calcium supplementation alone is not correlated with bone health and does not prevent bone fractures – but supplementing with vitamin D does
• This 2007 meta-analysis in the Journal of Clinical Nutrition showed that calcium supplementation did not reduce fracture rates in older women.
• This 2014 study showed that calcium supplementation does not prevent bone fractures in postmenopausal women.
• This 2016 meta analysis showed that calcium in conjunction with vitamin D reduces the risk of hip fractures by 30%
Calcium supplementation alone does not prevent fractures in the elderly, but combining it with vitamin D does. Calcium is the dominant mineral in bone, and vitamin D is important for the efficient absorption of calcium and for effective functioning of bone cells.
2. Low calcium may not be the problem
The problem we will address here is low bone mineral density. A common misconception is if bone density is low, there must be a lack of calcium and so calcium must be low – so we must supplement! This happens in some cases, and not in others. Some people may have a problem in HOW the calcium is being moved around in the body. Normally, calcium is constantly being RESORBED and RE-ABSORBED from bone without any net effect. The bone stays strong.
It is a delicate balance controlled by the hormones parathyroid hormone (PTH) and calcitonin. And many factors contribute to either bone formation or resorption, as seen in the image below. With age and especially after menopause in women due to rapidly declining estrogen levels, this fine balance may tip towards more bone resorption. This causes high calcium levels in the blood, which leads to lower absorption of calcium from the intestines. Your body thinks it has enough calcium, so it rejects any more calcium. In fact, during the 5 years right after menopause, it is NOT recommended to supplement calcium for this reason. You may be putting more and more calcium in your system, but your body will reject it. However, AFTER 5 years of menopause, calcium supplementation becomes beneficial and may reduce bone loss by up to 1% per year.
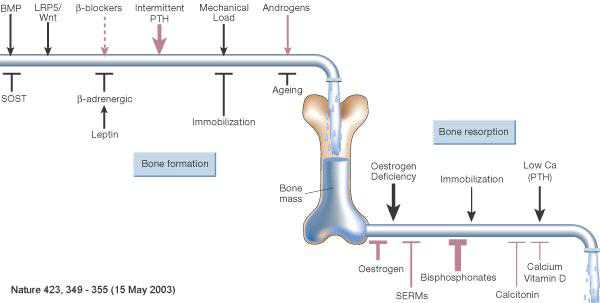
It is best to discuss with your doctor if any of the above factors are affecting your bone health before supplementing calcium. Bone health is not just about how much calcium you have in your body.
3. Too much calcium may be harmful
Adding to the above point, if someone has a higher rate of resorption (aka calcium mobilized out of bone) this may cause higher calcium levels in the bloodstream. This circulating calcium may then contribute to calcification of arteries or atherosclerosis. Would you want to add more calcium through supplementation in this case? Not a good idea. Have your calcium serum levels checked with your doctor before supplementing calcium.
Furthermore to support this theory, a few studies have shown that calcium supplementation can increase risk of heart attacks and strokes compared to those who don’t supplement:
- This 2008 British Medical Journal (BMJ) study found higher cardiovascular events including heart attacks and strokes in healthy postmenopausal women who took calcium supplements.
- Another 2012 BMJ study of 24,000 people found that those taking calcium supplements had a 139% greater risk of heart attacks during the 11-year study (calcium-rich foods did not increase the risk).
- This 2010 BMJ meta-analysis found that calcium supplements increased the risk of heart attack by 31%, stroke by 20%, and death from all causes by 9%.
- This 2013 JAMA study showed in 12,000 men that calcium supplementation increased the risk of death from heart disease by 20%. Dietary intake of calcium was not associated with any reported risks.
More recent analyses show conflicting results.
- A 2015 meta-analysis shows that calcium 500 mg per day or more, taken alone or along with vitamin D, does NOT increase the risk of myocardial infarction in postmenopausal women.
- Another meta-analysis published in 2016 shows that calcium intake, alone or along with vitamin D, is not associated with increased risk of cardiovascular disease in adults when used in amounts that are within tolerable upper intake levels (2000-2500 mg per day).
All in all, there is no consensus on whether calcium supplementation increases cardiac risk. Until more is known, it is safe to make sure calcium intake stays below the upper tolerance level, and to take it with vitamin D.
Another thing to consider is whether or not calcium is contaminated with lead. In nature, lead and calcium stick together. So consider this: if cows have lead in their feed, it will end up in their bones. For this reason, I discourage bone broth as a source of calcium. A 2013 study questioned the safety of bone broth, showing that even when made from organic bones, it could have significant amounts of lead. Lead is harmful to the brain, kidneys, and blood vessels. Calcium supplements from unrefined calcium carbonate also have the highest level of lead contamination according to this study.
4. Calcium needs cofactors to be absorbed
Your body cannot use isolated calcium. Unless it is attached to cofactors (other vitamins and minerals), calcium is not bioavailable and may be harmful as I explained earlier. When consumed in proper balance with its cofactors, it is very vital. Calcium should be ingested as a team with these cofactors:
- Vitamin D acts like a hormone in the body and helps the body absorb and utilize calcium. Many studies have now shown that in order to be beneficial, calcium must be taken with vitamin D. Keep in mind that vitamin D production is affected by aging. People over 65 years of age need 2-3 times the amount of vitamin D because their skin only produces about a quarter as much vitamin D as the skin of adults in their 20s or 30s.
- Vitamin K2 activates the protein called osteocalcin in bones which allows the bones to “hold on” to calcium. It also protects the arteries from calcium deposits. A higher intake of K2 (especially MK-7) is correlated with a significant reduction in heart disease and bone fractures (source). I recommend reading more about the importance of vitamin K2 in the book Vitamin K2 and the Calcium Paradox: How a Little-Known Vitamin Could Save Your Life written by a naturopathic doctor. Food sources of K2 include eggs, fermented foods, natto, kale and spinach.
Fun fact: Natto, a fermented soybean product is the only non-animal source of K2.
- Magnesium is needed in balance with calcium for heart health and proper muscle function. Calcium supplementation may actually deplete magnesium and it tends to already be low in most people. You can get magnesium from adzuki beans, pumpkin seeds, and almonds.
5. Food is the best source of calcium
At the end of the day, the best way to optimize calcium levels is through diet. After all, humans have been building strong bones without supplementation since the beginning of existence.
Dairy products (grassfed) – dairy is still the best source of dietary calcium and vitamin K2, but there are things we have to be careful about. Dairy from factory farmed cows has very low vitamin K2 and other fat soluble vitamins. The pasteurization and homogenization makes it difficult to digest. Some people are intolerant to dairy, so watch out as it can cause an inflammatory response, which is not healthy for bones. Seek out aged cheeses, grassfed ghee, grassfed butter and raw milk for the most calcium and nutrients.
Leafy greens – Kale, dandelion, turnip greens, mustard greens, swiss chard, bok choy, spinach and collard greens are good sources of calcium. Keep in mind however that leafy greens have calcium, but some are also high in oxalates, which block the absorption of this mineral. Broccoli, kale, and mustard greens are free of oxalates, so calcium from these vegetables is absorbed by up to 65%. Serve leafy greens with a source of vitamin K2, such as pastured eggs, melted butter or ghee.
Blackstrap molasses – You can use this as a substitute for sugar. A tablespoon contains 8% of the daily value of calcium.
Canned seafood – Canned sardines and canned salmon (with bones) are excellent sources of calcium. If you haven’t eaten these options before, don’t let that turn you off – the bones are barely noticeable in texture.

Black eyed peas and white beans– Although legumes can be difficult to digest for some people, they can be a good source of calcium.
Calcium fortified foods – non dairy milks, orange juice, cereals, various bread products.
The absorption rate of calcium from cow’s milk, calcium-set tofu, and fortified nut milks is about 30%.
6. If you’re going to take a supplement – take this form…
The main types of calcium include calcium carbonate (like Tums), coral calcium and algae-derived calcium, bone-derived calcium (like bone broths, MCHC and Bone Up) and calcium chelates (like calcium citrate, calcium lactate and calcium malate).
Calcium carbonate is one of the most common types of calcium found in supplements, either by itself or in combination with other types. It is low cost and is the most concentrated form, requiring less pills. Unfortunately, it seems to be the worst in causing cardiovascular plaque growth in populations most at risk, harder to digest and has the highest lead contamination.
The best form of calcium are chelates (like calcium citrate and malate). They are better absorbed regardless of digestive function and can be taken with or without food. They also do not compete with iron absorption like other types of calcium. And they are low in lead and least apt to cause calcification.
Bottom Line
- Calcium plays an important role in bone health
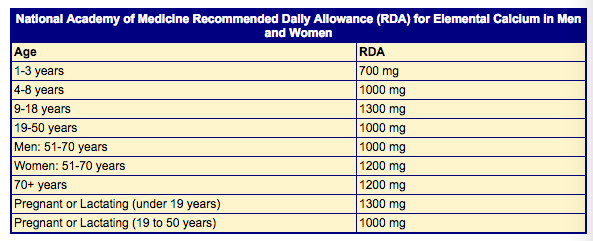
- Calcium daily dose of 500–700 mg can easily be obtained from food alone. A diet tracking website or app like myfitnesspal.com can help you calculate how much calcium you are getting from food, and calcium supplements should only cover any shortfall until you reach the daily recommended dose (for women over 50, this is 1200mg/day). Do not take any more calcium than the recommended amount.
- To optimize absorption, total daily calcium should be divided throughout the day into individual 500mg doses, regardless of the dose. Anything above this has a risk of lodging into your blood vessels.
- Calcium CITRATE or MALATE forms are especially bioavailable and better than carbonate (those chalky Tums). It may be a bit more expensive, but it is better broken down in the stomach, has a lower risk of contamination and has a lower chance of causing kidney stones. Citrate binds to oxalate, reducing its intestinal absorption.
- High serum calcium levels, known as hypercalcemia, has been associated with an increased risk of cardiovascular events, myocardial infarction, and stroke. It is best to have your serum calcium levels checked with your doctor before supplementing.
- Take calcium together with its co-factors: vitamin D, vitamin K, and magnesium.
- Get your vitamin D levels tested to see if they are in the optimum range. Adequate levels of vitamin D will help absorb calcium from foods and supplements.
- If you’re looking to strengthen bones, it is also important to perform load-bearing exercise or resistance training. In fact, dietary calcium regardless of the source, will probably not strengthen bones if such exercise is not achieved. Walking and running is also good since the stimulation of bones in the legs/ankles/feet stimulates other bones in the body to add calcium.
This article is for educational purposes only and does not advocate self-diagnosis. Due to individual variability, consultation with a licensed health professional, such as a naturopathic doctor is highly recommended prior to starting a natural treatment plan.

0 Comments Leave a comment